

Importance of oral sensory and motor stimulation in tube-fed children

Viviane Cappellari
DHA License Number: 00082911-001
Head of Speech & Language Department
MS, SLP
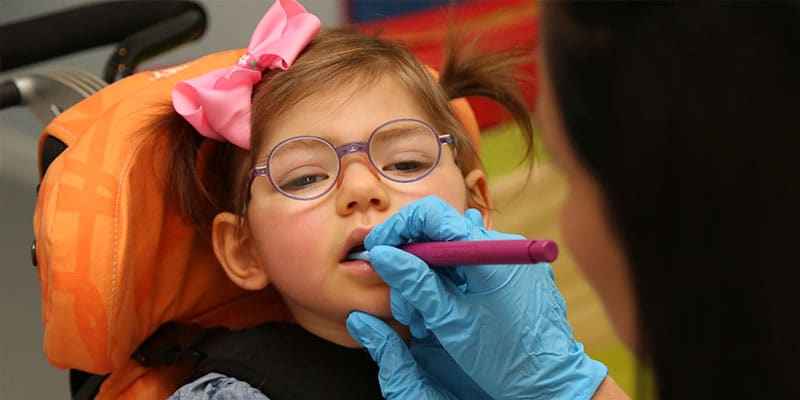
A feeding tube is a medical device that is necessary when an individual cannot take food, fluids, or medication by mouth safely. This difficulty may be due to an inability to suck, chew, or swallow, or any other issues that make eating challenging and increase the risk of choking and aspiration of food or fluids. It is often used in Neonatal Intensive Care Units (NICU) to support growth and weight gain in term or preterm babies who may struggle with muscle strength, immature suck-swallow reflex (not being able to coordinate the sequence of movements), neurological disease, respiratory distress, cardiopathic disorders, abdominal or gastrointestinal defects, problems with electrolyte imbalances/elimination, or when slow or irregular weight gain patterns for non-specific reasons are observed(1, 2).
There are several types of feeding tubes, some of which are designed for short-term use, like Nasogastric Tube- NG tube and Nasojejunal tube – NJ, while others are for a long-term or even permanent use, like the Percutaneous Endoscopic Gastrostomy (PEG) or Gastric Tube -G-Tube. Some children may start being fed on an Naso-gastric tube during their time in the NICU and after their discharge from the hospital, they still may require to be partially or totally fed on the tube due to neurological or medical reasons.
Parents are usually concerned about when their baby’s tube will be removed. Criteria for transition from tube to oral feeding may vary according to the doctor or the hospital. In general, weight gain without supplementation by tube feeding is one of the major criteria for a successful transition regarding premature babies. However, the transition from tube to oral feeding may in some cases take only several days or weeks while in others, it can be more challenging, lasting for months or even years. In children with neurological disorders, tube feeding can be a lifelong necessity.
Irrespective of the expected duration of tube feeding, an action plan and a multidisciplinary approach are required at the outset to help the child reach either full oral feeding at the earliest possible or partial oral feeding along with tube feeding support. A long-term use of tube feeding in the absence of any medical need can cause tube dependency, as the child may develop oral aversion or exhibit a lack of oral motor strength. Oral sensory and motor therapy along with nutritional adjustments are crucial to avoid tube dependency and decrease chances of oral aversion. It also helps to keep mobilizing oral structures, strengthening the muscles involved in the oral functions(3).
Babies or children need to gradually receive oral stimulation along with tube feeding as soon as the tube is placed, even when the child is still in the NICU. A variety of techniques can be performed to promote oral sensory and motor stimulation, which will lead to feeding-like movements such as sucking, chewing, and swallowing. As the child’s sensory system responds to such non-nutritive stimulation, food can be introduced following controlled feeding techniques in the absence of any signs of discomfort or respiratory distress. It is important then to expose the child to different flavors and textures. Consistencies will be managed according to the child’s motor and sensory responses, improving oral functions like chewing, sucking, and swallowing. Several studies have noted the benefits of allowing infants in NICUs to suck on a pacifier, which is classified as a non-nutritive sucking, during tube feedings(4). The results revealed that infants who were encouraged to suck on pacifiers needed tube feeding for a shorter time than those who did not receive any oral simulation, started bottle feeding or adaptive feeding earlier, and were discharged from hospital earlier. In addition, Bernbaoun et al.(4) demonstrated that non-nutritive sucking among babies decreased intestinal transit time, reduced constipation, and presented faster weight gain. In the same way, other studies have shown that promoting sucking while tube feeding can lead to decreased restless states(5).
Bazyk’s(6) study describes children with multiple complications related to digestive, cardiac, or respiratory systems who were more prone to lengthy feeding transitions. He found that prematurity was not as relevant as the presence of multiple medical complications in the weaning off tube, which means that children with complex needs may require to stay longer on tube feeding. The study also highlights that children with complex medical conditions are more prone to developing hypersensitivity to any stimuli in their mouth, due long hospitalization and unpleasant medical procedures.
Parents face considerable uncertainty when they get to know that their child requires tube feeding. Concerns regarding aspiration, respiratory, or cardio issues make them afraid of providing their child any oral feeding experience The therapy team needs to train parents on providing gradual oral stimulation to the child since the start of the tube feeding journey. For children who are on a long-term tube feeding plan, parents should also be guided to involve their child in a meal-time environment that provides social-feeding interaction will all family members and stimulates the senses around food (sight, smell, and sound), which will lead to a positive perception about food(7,8).
A well-trained and experienced speech and language therapist, specialized in dysphagia/ feeding and oral motor, is the best professional to support weaning off tube feeding or promoting maximum oral feeding, even in children who will tube-fed for the long-term. A feeding therapist may use different types of oral sensory stimulation and controlled feeding techniques. However, as previously mentioned, a multidisciplinary approach is necessary. Professionals such as gastroenterologists, pediatricians, occupational therapists, psychologists, and pulmonologists play a critical role in helping the child reach full or maximum possible oral feeding.
If your child is currently or was tube fed and you have questions about their oral feeding, please contact our team. Our professionals are qualified to assess and treat children who need support in transitioning from tube to oral feeding, and those who have a long-term tube feeding indication and require oral sensory and motor stimulation to maintain oral feeding.
Sources:
- Sarah J. Mason, MSc, 1.2 Gillian Harris, PhD, CPsychological, 1.2 and Jaqueline Blisset, PhD, CPsychol1. (2005) Tube feeding in Infancy: Implications for development of normal eating and drinking skills. Dysphagia 20 46-61.
- Abdelhadi et al. (2020) Transition from nasogastric feeding tube to gastrotomy tube feeding in pediatric patients: A survey on Decision-Making and Practice. Nutr in Clinical Practice V 00 N 0. 1-11.
- Kron H., Winter P. Kinderman (2017) development, prevention, and treatment of feeding tube dependency. Eur JPediatr 176. 683-688.
- Bernbaum JC, Pereira GR, Watkins JB, Peackhan GJ (1983): Nonnutritive sucking during gavage feeding enhances growth and maturation in premature infants. Pediatrics 71: 41-45.
- Di Pietro JA, Cusson RM, Caughy MO, Fox NA (1994): Behavioral and psychologic effects of nonnutritive sucking during gavage feeding in preterm infants Pediatr Res 36: 207-214.
- Guttrand F, Sullivan PB (2010) Gastrotomy tube feeding: when to start, how to feed and when tostop. Eur.J clin Nutr 64 (Suppl 1): S17-S21.
- Morag I, Hendel Y, Karol D, Geva R, Tzipi S. (2019): Transition from Nasogastric Tube to Oral feeding: The role of parental guided responsive feeding. Front in Peadiatr. V. 7 190.


