

The integrated Physical Therapy and Speech and Language Therapy teamwork for children with neurological conditions

Priscila Cunha Santos
DHA License Number: 26093763-001
Senior Pediatric Physical Therapist
Neurology and Neuroscience, PhD
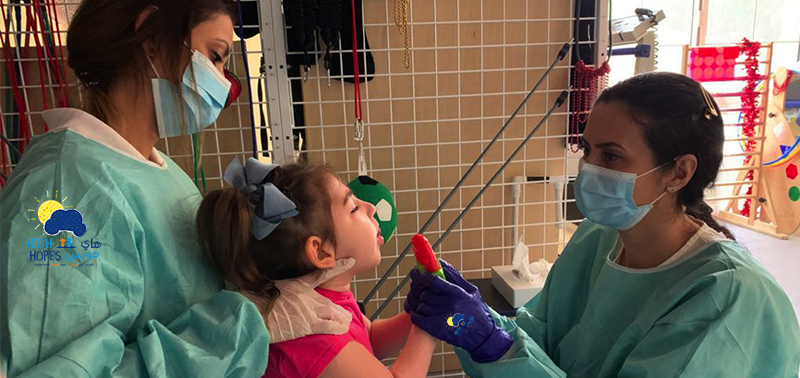
The demands of children’s neurological rehabilitation are related to autonomy and independence, and often involve contributions from several disciplines, such as the physical therapist, speech and language therapist, occupational therapist, vision specialist, and psychotherapist, among others. Individualized actions of each discipline may bring specific benefits to each area, but it does not necessarily mean that the child will be able to integrate skills to stablish efficient and natural function.
There are many studies in the therapy field advocating for the benefits of working as a team to enhance functions and achieve comprehensive results in individuals with neurological disorders. Over the past few years, researches have demonstrated a strong connection between Physical and Oral Motor therapy, based on a correlation between postural control and the stomatognathic system, establishing reciprocal influence between corporal positioning and oral motor structures and functions. (Alghadir et al., 2014, 2015a, 2015b)
Some children with neurological disorders may have oral motor functions affected since birth. These effects may include difficulties in sucking, swallowing, chewing, breathing and speaking. Consequently, these children often display structural and myofunctional disorders such as an oblong face, narrow and high hard palate, shortened upper lips and hypotonic, everted lower lips, an opened-mouth posture, malocclusion, tongue and jaw protrusion, and poor neck and head control. All of these combined features have a direct impact on the body’s center of gravity. These all may cause a sort of chain reaction affecting and contributing to oro-myofunctional disorders and reducing postural control. In addition, symptoms of oropharyngeal dysphagia, which is the difficulty or inability in swallowing saliva, secretions and food, are frequently associated with respiratory problems such as bronchopneumonia due to aspiration and ineffective coughing. Apart from this, the oral breathing pattern and neck extension reduce the strengthening of the abdominal muscles and phonatory control. Reduced expiratory muscle strength may negatively affect the child’s ability to generate adequate expiratory pressure for voice production, which limits the possibilities of verbal communication, and also result in ineffective cough, placing the child at risk of not being able to clear the airway if aspiration occurs. (Brooks, McLaughlin & Nora Shields, 2017)
The question is… “How can professionals from different disciplines such as Physical and Speech and language therapy integrate goals and strategies?”
There are many ways to work as a team: a Multidisciplinary approach, an Interdisciplinary or Transdisciplinary approach. A quite well-known modality, the Multidisciplinary approach is when a team of professionals works together to promote the child’s development, not necessarily under the same roof. They do this by sharing knowledge and discussing goals, but not targeting common goals. The Interdisciplinary approach is when professionals, under the same roof, set strategies aiming to integrate goals from more than one discipline and boost results. Although professionals may integrate goals and even can join the same session, each therapist has a well-defined role restricted to their area of knowledge. In this approach therapist’s roles are divided but applied in synchrony during the session, and this can provide a practical blend between resource investment and patient outcomes.
A more complex approach is known as the Transdisciplinary approach. It is described as a very family and child-centered approach, where team members are committed to teach, learn, and work together to implement coordinated services. It saves time of the child and family by reducing required sessions, by combining goals and crossing over disciplines. However, the transdisciplinary approach can be difficult to implement effectively because it requires intensive planning and monitoring on the part of the therapy team. Therapists are highly trained and guided to integrate strategies and therapeutic actions from another discipline, e.g. after thorough consultation with the Speech therapist regarding the child’s needs, a physical therapist (PT) may apply strategies to promote verbal communication during PT sessions, and then report progress to the speech and language therapist. In this case, the professional who applies this approach is capable not only of applying the stimulus, but also of understanding the goals, and qualifying, quantifying and reporting the results to the specialized therapist for further discussions on the next steps (King G at all, 2009).
With the development of the International Classification of Functioning, Disability and Health (ICF) by the World Health Organization (WHO, 2001) to meet the functional demands of patients, health professionals were directed to approach patients in all aspects related to their lives, considering the individual’s body structures and functions, as well as the environment this person is inserted in and the active participation of daily routine and social interactions. It became necessary for each professional, regardless of their specialty within the rehabilitation team, to understand and approach the patient in a broad way in order to meet their functional demands. This approach does not aim to replace a therapist in the team in any circumstance, but seeks to combine knowledge and action for more comprehensive results.
Indications and benefits
The PT and SLT Interdisciplinary and Transdisciplinary approaches are very useful for the child who has speech or feeding issues associated with postural control dysfunction and gross motor development delay, such as cerebral palsy, hypotonic syndromes and neuromuscular diseases.
Integrating goals to improve feeding skills and align the body’s center of gravity can also improve some oral motor issues. For example, oral-motor exercises to improve chewing are proven to promote jaw stability, which in turn generates more head stability, postural alignment, breath coordination and core muscle strength.
In general, the Transdisciplinary approach may promote a number of benefits including increased service efficiency, reduction in cost of services, more effective and direct parent guidance, more coherent intervention plans and holistic service delivery, and more opportunities for professionals to learn from each other.
Independent of which approach is adopted, a team of therapists has the responsibility of maintaining professional enrichment, by engaging with leaning opportunities in the areas that affect their work. Therapists should be open to learning about strategies related to their primary discipline, supported by the rest of the team.
If you want to know more about our Physical Therapy and Speech & Language Therapy Interdisciplinary and Transdisciplinary approach, feel free to contact us.
Blog is written by:
Viviane Cappellari and Priscila Cunha Santos
Sources:
- King G at all (2009). The Application of a Transdisciplinary Model for Early Intervention Services. Infants & Young Children, Vol. 22, No. 3, pp. 211–223
- Alghadir A, Zafar H, Whitny SL, Iqbal Z. (2014) Effect of chewing on postural stability during quiet standing in healthy young males. Somatosensory & Motor Research, DOI: 10.3109/08990220.2014.969837.
- Alghadir A, Zafar H, Iqbal Z. (2015a) Effect of tongue position on postural stability during quiet standing in healthy young males, Somatosensory & Motor Research, DOI: 10.3109/08990220.2015.1043120.
- Alghadir A, Zafar H, Iqbal Z. (2015b) Effect of three different jaw positions on postural stability during standing. Functional Neurology, 30(1): 53-57.
- Brooks M, McLaughlin E, Shields N. (2017) Expiratory muscle strength training improves swallowing and respiratory outcomes in people with dysphagia: a systematic review, International Journal of Speech-Language Pathology, DOI: 10.1080/17549507.2017.1387285.


